Trusted Nutrition Information and Support

What is Celiac Disease?
Celiac disease is an immune-mediated disorder in which eating gluten causes damage to the small intestine in those who are genetically predisposed.
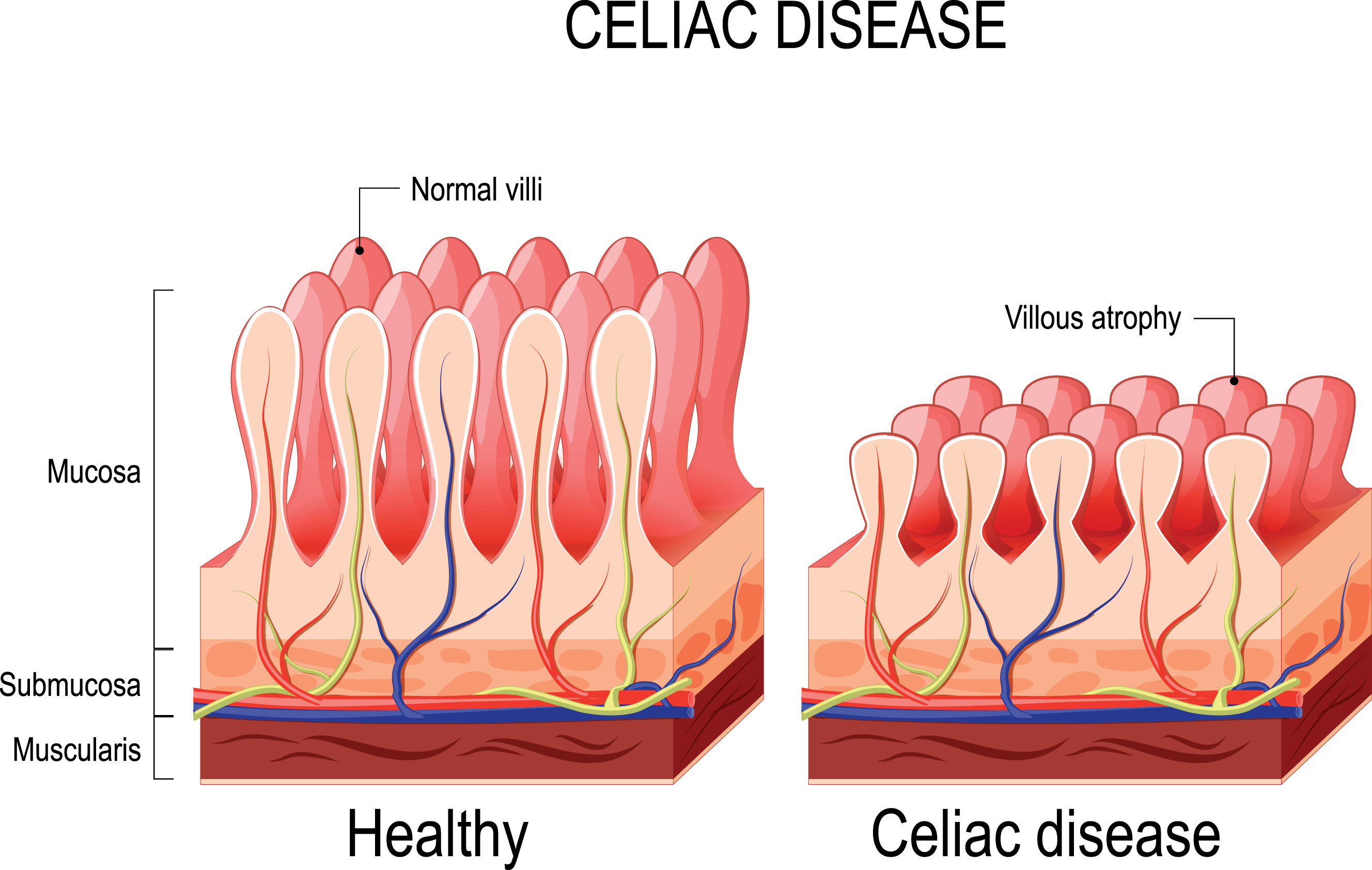
Why Does Nutrition Matter in Celiac Disease?
Nutrition is central to managing celiac disease because it is both the treatment and the key to healing and long-term health. Unlike many conditions where diet can play a supportive role, nutrition in celiac disease isn’t supportive care, it is the treatment.
Learn More Details about Celiac Disease
Even tiny amounts of gluten can cause harm to the small intestine, even if the person may not feel symptoms. While symptoms of celiac disease can affect the digestive system or other organs, some people with the condition are asymptomatic (show no symptoms). Regardless of the presence of symptoms, all people with celiac disease are at risk of long-term complications.1,4
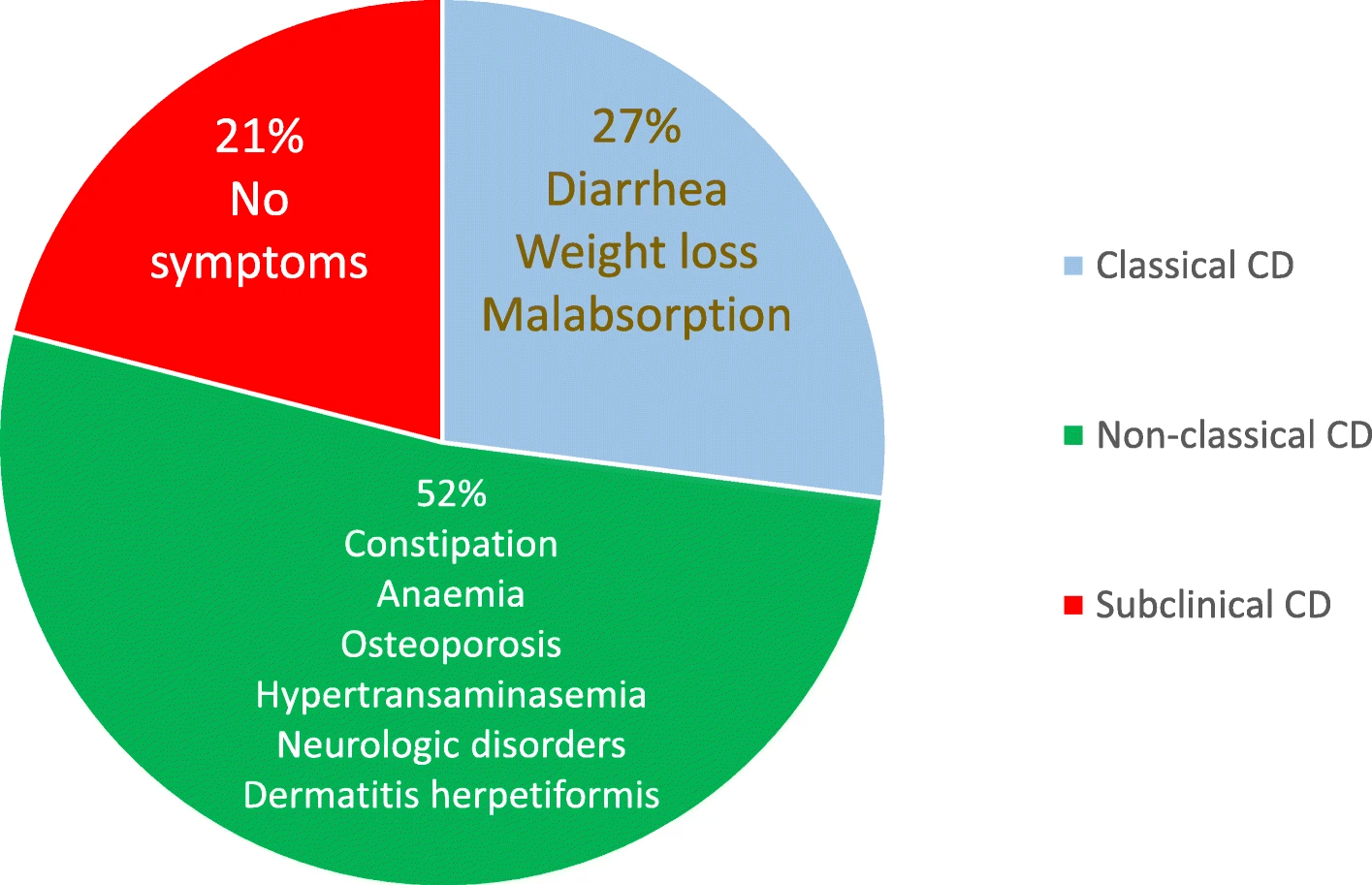
Caio G, Volta U, Sapone A, et al. Celiac disease: a comprehensive current review. BMC Med. 2019; 17(1):142. doi: 10.1186/s12916-019-1380-z. Distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/).
Non-celiac gluten/wheat sensitivity (NCGWS) affects up to 10% of adults worldwide. While people with NCGWS experience symptoms similar to those of celiac disease, they do not test positive for celiac disease.6
True gluten reactivity is uncommon and typically mild. Symptoms after gluten intake in individuals without celiac disease or wheat allergy are real, but may be explained by:7
- Fermentable carbohydrates (fructans), which are found in wheat and its derivatives
- The expectations and beliefs that gluten is harmful
The diagnosis of celiac disease is typically made by combining:8,9
- Celiac disease serology (blood) tests: TTG IgA antibody and total IgA level
- Small intestinal biopsies: remain the diagnostic gold standard for celiac disease
- HLA DQ 2,8 genetic testing
The North American Society For Pediatric Gastroenterology, Hepatology & Nutrition (NASPGHAN) recommends eating roughly 2 servings of gluten, equivalent to 2 slices of wheat-based bread, daily for 6-8 weeks prior to testing.11
Please consult with your gastroenterologist regarding your gluten challenge and never undertake it when pregnant.11
Avoiding gluten is currently the only way to prevent small intestinal damage and relieve the various symptoms of the disease.
While the gluten-free diet is challenging to follow and has a negative impact on daily quality of life,12, with the support of an expert dietitian, it can be properly followed without nutritional deficiencies and can allow for a joyful quality of life.
The best way to know if a food contains gluten is by reading the ingredients list.

Sources of gluten
Gluten-containing grains and their derivatives include:13
- Wheat
- Derivatives of wheat: wheatberries, durum, emmer, semolina, spelt, farina, farro, graham, Kamut® khorasan wheat, einkorn wheat
- Barley
- Rye
- Triticale
- Malt
Common foods containing gluten are:13
- Pastas
- Noodles
- Breads and pastries
- Crackers
- Baked goods
- Corn flakes
- Granola
- Breakfast foods
- Breading and coating mixes
- Croutons
- Flour tortillas
- Brewer’s yeast
Unexpected sources of gluten
Gluten is also found in some unexpected foods:13
- Chocolates, candies, and ice creams
- Seasoning mixes
- Condiments and salad dressings
- Processed meats
- Meat substitutes
- Oats
- Soy sauce
- Potato chips and French fries
- Alcohol and other beverages (dessert wines, beers, ales, lagers, maltbeverages)
- Malt vinegars
- Soups and gravies
While not all variations of these foods contain gluten, some do. Therefore, look for a gluten-free claim and read the ingredient list. Please refer to the Celiac Disease Foundation list of sources of gluten for more information.
The goal of a gluten-free diet is to choose naturally gluten-free staples rather than replacing every gluten-containing food with a processed version. Learn more about the benefits of following a Mediterranean diet with naturally gluten-free foods.
Gluten-free substitutes are becoming common, but they are more expensive, contain less protein and dietary fiber, and higher unhealthy fats and salt than their gluten-containing counterparts.14,15,16 The high amount of food additives in gluten-free ultraproccessed foods may harm gut health and the microbiome.17
Also, just because a product is labelled gluten-free or lactose-free, it does not mean it is necessarily low in fermentable carbohydrates (FODMAPs). If you are on a low FODMAP diet for managing IBS symptoms, please check the ingredient list first.18
While the gluten-free diet should be reviewed in detail with the guidance of a GI expert dietitian, many people do not have access to the support of a dietitian to help them plan a balanced, gluten-free diet. Find a gastroenterology-expert dietitian in your area.
Considering the impact of this restrictive diet on the overall quality of life and emotional well-being, working with a GI psychologist is highly recommended.
New treatments could be on the horizon that could ease the quality of life of people with celiac disease, especially those 30% of sufferers who still have symptoms despite avoiding gluten. Some potential therapies target different steps in the disease pathway involve:
- Enzymes that improve the digestion of gluten, breaking it down into smaller, less harmful fragments.21
- Boosting the small intestine barrier so it is more difficult for partially digested gluten to access the bloodstream.22
- Administer oral or small intestine bacteria that can metabolize gluten.23
- Targeting the gut lining to attenuate the immune reaction to gluten.24
- Targeting the immune system to prevent it from damaging the intestine in response to gluten.25
Even tiny amounts of gluten can cause harm to the small intestine, even if the person may not feel symptoms. While symptoms of celiac disease can affect the digestive system or other organs, some people with the condition are asymptomatic (show no symptoms). Regardless of the presence of symptoms, all people with celiac disease are at risk of long-term complications.1,4

Caio G, Volta U, Sapone A, et al. Celiac disease: a comprehensive current review. BMC Med. 2019; 17(1):142. doi: 10.1186/s12916-019-1380-z. Distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/).
Non-celiac gluten/wheat sensitivity (NCGWS) affects up to 10% of adults worldwide. While people with NCGWS experience symptoms similar to those of celiac disease, they do not test positive for celiac disease.6
True gluten reactivity is uncommon and typically mild. Symptoms after gluten intake in individuals without celiac disease or wheat allergy are real, but may be explained by:7
- Fermentable carbohydrates (fructans), which are found in wheat and its derivatives
- The expectations and beliefs that gluten is harmful
The diagnosis of celica disease is typically made by combining:8,9
- Celiac disease serology (blood) tests: TTG IgA antibody and total IgA level
- Small intestinal biopsies: remain the diagnostic gold standard for celiac disease
- HLA DQ 2,8 genetic testing
The North American Society For Pediatric Gastroenterology, Hepatology & Nutrition (NASPGHAN) recommends eating roughly 2 servings of gluten, equivalent to 2 slices of wheat-based bread, daily for 6-8 weeks prior to testing.11
Please consult with your gastroenterologist regarding your gluten challenge and never undertake it when pregnant.11
Avoiding gluten is currently the only way to prevent small intestinal damage and relieve the various symptoms of the disease.
While the gluten-free diet is challenging to follow and has a negative impact on daily quality of life,12 with the support of an expert dietitian, it can be properly followed without nutritional deficiencies and can allow for a joyful quality of life.
The best way to know if a food contains gluten is by reading the ingredients list.

Sources of gluten
Gluten-containing grains and their derivatives include:13
- Wheat
- Derivatives of wheat: wheatberries, durum, emmer, semolina, spelt, farina, farro, graham, Kamut® khorasan wheat, einkorn wheat
- Barley
- Rye
- Triticale
- Malt
Common foods containing gluten are:13
- Pastas
- Noodles
- Breads and pastries
- Crackers
- Baked goods
- Corn flakes
- Granola
- Breakfast foods
- Breading and coating mixes
- Croutons
- Flour tortillas
- Brewer’s yeast
Unexpected sources of gluten
Gluten is also found in some unexpected foods:13
- Chocolates, candies, and ice creams
- Seasoning mixes
- Condiments and salad dressings
- Processed meats
- Meat substitutes
- Oats
- Soy sauce
- Potato chips and French fries
- Alcohol and other beverages (dessert wines, beers, ales, lagers, maltbeverages)
- Malt vinegars
- Soups and gravies
While not all variations of these foods contain gluten, some do. Therefore, look for a gluten-free claim and read the ingredient list. Please refer to the Celiac Disease Foundation list of sources of gluten for more information.
The goal of a gluten-free diet is to choose naturally gluten-free staples rather than replacing every gluten-containing food with a processed version. Learn more about the benefits of following a Mediterranean diet with naturally gluten-free foods.
Gluten-free substitutes are becoming common, but they are more expensive, contain less protein and dietary fiber, and higher unhealthy fats and salt than their gluten-containing counterparts.14,15,16 The high amount of food additives in gluten-free ultraproccessed foods may harm gut health and the microbiome.17
Also, just because a product is labelled gluten-free or lactose-free, it does not mean it is necessarily low in fermentable carbohydrates (FODMAPs). If you are on a low FODMAP diet for managing IBS symptoms, please check the ingredient list first.18
While the gluten-free diet should be reviewed in detail with the guidance of a GI expert dietitian, many people do not have access to the support of a dietitian to help them plan a balanced, gluten-free diet. Find a gastroenterology-expert dietitian in your area.
Considering the impact of this restrictive diet on the overall quality of life and emotional well-being, working with a GI psychologist is highly recommended.
New treatments could be on the horizon that could ease the quality of life of people with celiac disease, especially those 30% of sufferers who still have symptoms despite avoiding gluten. Some potential therapies target different steps in the disease pathway involve:
- Enzymes that improve the digestion of gluten, breaking it down into smaller, less harmful fragments.21
- Boosting the small intestine barrier so it is more difficult for partially digested gluten to access the bloodstream.22
- Administer oral or small intestine bacteria that can metabolize gluten.23
- Targeting the gut lining to attenuate the immune reaction to gluten.24
- Targeting the immune system to prevent it from damaging the intestine in response to gluten.25
Delicious and Nutritious Recipes
Search Our Resource and Lifestyle Database
Gain Knowledge with Our Research
References
- Doyle JB, Silvester J, Ludvigsson JF, et al. Advances in the pathophysiology, diagnosis, and management of celiac disease. BMJ. 2025; 391:e081353. doi: 10.1136/bmj-2024-081353.
- Karimzadhagh S, Abbaspour E, Ghodous S, et al. Global prevalence and clinical manifestations of celiac disease among first-degree relatives: a systematic review and meta-analysis. Am J Gastroenterol. 2024; 120(7):1488-1501. doi: 10.14309/ajg.0000000000003227.
- Beyond Celiac. What is celiac disease? Available: https://www.beyondceliac.org/celiac-disease/
- Celiac Disease Foundation. Symptoms of celiac disease. Available: https://celiac.org/about-celiac-disease/symptoms-of-celiac-disease/
- Caio G, Volta U, Sapone A, et al. Celiac disease: a comprehensive current review. BMC Med. 2019; 17(1):142. doi: 10.1186/s12916-019-1380-z.
- Shiha MG, Manza F, Figueroa-Salcido OG, et al. Global prevalence of self-reported non-coeliac gluten and wheat sensitivity: a systematic review and meta-analysis. Gut Published Online First: 28 October 2025. doi: 10.1136/gutjnl-2025-336304.
- Biesiekierski JR, Jonkers D, Ciacci C, et al. Non-coeliac gluten sensitivity. Lancet. 2025; 406(10518):2494-2508. doi: 10.1016/S0140-6736(25)01533-8.
- Rubio-Tapia A, Hill ID, Semrad C, et al. American College of Gastroenterology Guidelines update: diagnosis and management of celiac disease. Am J Gastroenterol. 2023; 118(1):59-76. doi: 10.14309/ajg.0000000000002075.
- Al-Toma A, Zingone F, Branchi F, et al. European Society for the Study of Coeliac Disease 2025 updated guidelines on the diagnosis and management of coeliac disease in adults. Par 1: diagnostic approach. UEGJ. 2025; doi: 10.1002/ueg2.70119.
- Sharma RR, Jansson-Knodell CL, Kumral D, et al. Evaluating for celiac disease in patients on a gluten-free diet: a practical approach. Am J Gastroenterol. 2025; 120(8):1676-1682. doi: 10.14309/ajg.0000000000003434.'
- Celiac Disease Foundation. Testing. Available: https://celiac.org/about-celiac-disease/screening-and-diagnosis/screening/
- Trott N, Holland W, Hoffmann O, et al. Food related quality of life and associations with demographic and clinical characteristics in people with coeliac disease. J Hum Nutr Diet. 2025; 38(3):e70051. doi: 10.1111/jhn.70051.
- Celiac Disease Foundation. Sources of gluten. Available: https://celiac.org/gluten-free-living/what-is-gluten/sources-of-gluten/
- Mehtab W, Agarwal S, Agarwal H, et al. Gluten-free foods are expensive and nutritionally imbalanced than their gluten-containing counterparts. Indian J Gastroenterol. 2024; 43(3):668-678. doi: 10.1007/s12664-024-01519-z.
- Myhrstad MCW, Slydahl M, Hellmann M, et al. Nutritional quality and costs of gluten-free products: a case-control study of food products on the Norwegian marked. Food Nutr Res. 2021; 65. doi: 10.29219/fnr.v65.6121.
- Lee AR, Wolf RL, Lebwohl B, et al. Persistent economic burden of the gluten free diet. Nutrients. 2019; 11(2):399. doi: 10.3390/nu11020399.
- Whelan K, Bancil AS, Lindsay JO, et al. Ultra-processed foods and food additives in gut health and disease. Nat Rev Gastroenterol Hepatol. 2024; 21(6):406-427. doi: 10.1038/s41575-024-00893-5.
- Barreirinhas S, Almeida C, Casal S, et al. Pre-packaged food targeted to gastrointestinal pathologies: are they low in FODMAP? Br J Nutr. 2025; 1-6. doi: 10.1017/S000711452510528X.
- AGA GI patient center. Celiac disease. AGA. Available: https://patient.gastro.org/celiac-disease/
- Kårhus LL, Skaaby T, Petersen J, et al. Long-term consequences of undiagnosed celiac seropositivity. Am J Gastroenterol. 2020; 115(10):1681-1688. doi: 10.14309/ajg.0000000000000737.
- Bonner ER, Tschollar W, Anderson R, et al. Review article: novel enzyme therapy design for gluten peptide digestion through exopeptidase supplementation. Aliment Pharmacol Ther. 2025; 61(7):1123-1139. doi: 10.1111/apt.70014.
- Damianos JA, Bledsoe A, Camilleri M, et al. Coeliac disease and the intestinal barrier: mechanisms of disruption and strategies for restoration. Gut. 2025; gutjnl-2025-335373. doi: 10.1136/gutjnl-2025-335373.
- Caminero A, Meisel M, Jabri B, et al. Mechanisms by which gut microorganisms influence food sensitivities. Nat Rev Gastroenterol Hepatol. 2019; 16(1):7-18. doi: 10.1038/s41575-018-0064-z.
- Rahmani S, Galipeau HJ, Clarizio AV, et al. Gluten-dependent activation of CD4+ T cells by MHC class II-expressing epithelium. Gastroenterology. 2024; 167(6):1113-1128. doi: 10.1053/j.gastro.2024.07.008.
- du Pré MF, Kleppa L, Dewan AE, et al. Peyer’s patch B cells sample transglutaminase-gluten complexes and drive celiac disease autoimmunity. Gastroenterology. 2025; 169(7):1450-1461. doi: 10.1053/j.gastro.2025.06.021.






%20%26%20Spinach%20Curry.jpg)



