New to IBD
Understanding IBD
Being diagnosed with IBD, whether Crohn’s disease or ulcerative colitis, can feel overwhelming. You may have questions about why this is happening, what to expect, and how to best manage it. Researchers continue to learn more about what causes IBD and how to treat it most effectively. Understanding what is happening inside the body, and how nutrition and lifestyle changes can help, is an essential step in playing an active role in your care.
Video created and shared by:
David L. Suskind, MD- Professor of Pediatrics, Division of Gastroenterology at Seattle Children's Hospital and founder of Nutrition in Immune Balance (NiMBAL)
Symptoms of IBD
The symptoms of IBD vary from person to person, but usually include:
- Persistent diarrhea
- Abdominal pain or cramping
- Rectal bleeding
- Unintentional weight loss
- Fatigue
- Stool urgency

Periods of “flare” (active disease) and remission often alternate, and symptoms fluctuate.
Without proper diagnosis and treatment, IBD can lead to serious complications such as:
- Bowel obstruction, especially in Crohn's disease, where inflammation can narrow the intestines.
- Malnutrition due to reduced appetite, poor nutrient absorption, or restrictive eating habits.
- Fistulas (abnormal connections between organs) and abscesses (local infections) mainly occur in Crohn's disease.
- An increased risk of colon cancer, especially with long-term ulcerative colitis.
- Inflammation in other parts of the body, such as the liver, joints, skin, and eyes.
How is IBD Diagnosed?
A diagnosis of IBD is made after assessing the patient's: medical history, physical examination, blood and stool tests, and, most importantly, the endoscopic picture (an intestinal examination using a flexible camera, such as during an endoscopy or colonoscopy) and histological picture (tissue examination under a microscope, usually from a small sample called a biopsy). Early diagnosis and effective treatment are essential to control IBD and prevent complications. Nutrition and lifestyle as part of treatment from the initial diagnosis can increase the chance of remission and reduce the development of complications. 1,2,3
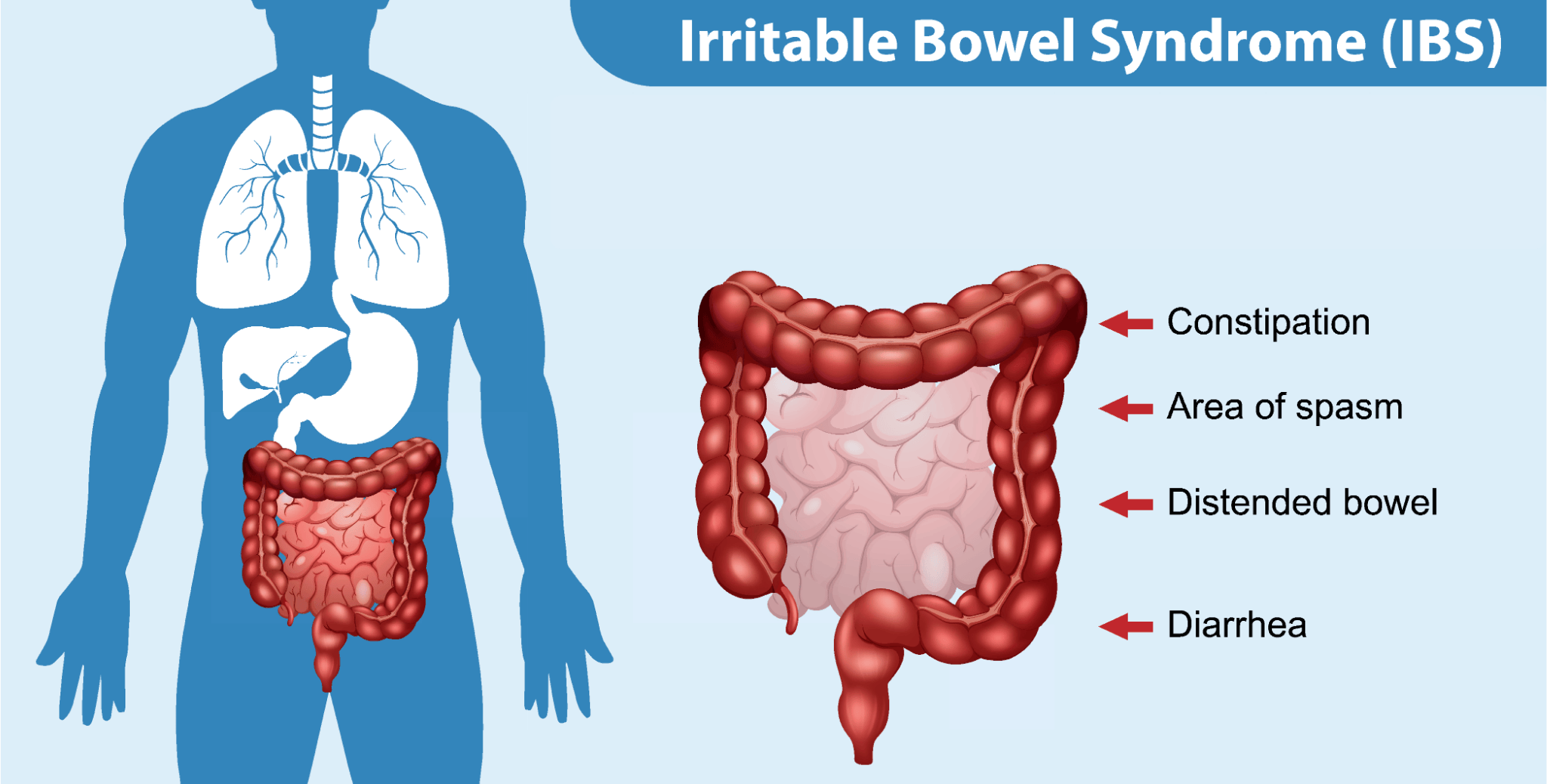
Is IBS the Same as IBD?
Irritable Bowel Syndrome (IBS) is a functional disorder of the gastrointestinal tract characterized by chronic abdominal symptoms and changes in bowel habits, such as diarrhea, constipation, or a combination of both. Living with unresolved IBS can be very distressing and debilitating, but does not cause visible inflammation or damage to intestinal tissue like IBD.
Although IBS and IBD are different conditions, they can overlap in certain ways:
- Shared symptoms: Both conditions can cause abdominal pain and changes in bowel habits.
- Coexistence: 30% of people with IBD who are in remission are also diagnosed with IBS.4
- Misdiagnosis: The early symptoms of IBD can sometimes resemble those of IBS, which can lead to a delay in proper diagnosis. Investigations such as measuring calprotectin or a colonoscopy with a biopsy are essential to distinguish between the two.
- Impact of stress: Stress can worsen the symptoms of both IBS and IBD.
Prevalence and Growth of IBD
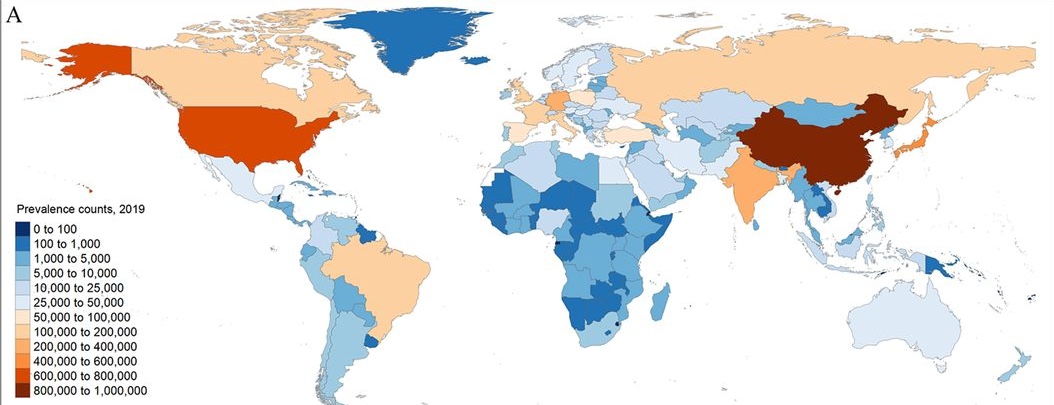
Health conditions are often described in terms of prevalence and incidence.
Prevalence- all existing cases at a given time (e.g., how many total people currently have IBD) Incidence- new cases over time (e.g., how many new people get IBD this year)
In 2019, it was estimated that 4.9 million people worldwide had IBD, with the rates steadily increasing. The number of people with IBD is also increasing in countries where a more Western lifestyle has recently been adopted. Studies show that people who migrate from a low-incidence area to a high-incidence area have a higher chance of developing IBD.10 The age at which most people develop IBD is between 20 and 30, with it being slightly more common in women.5
Mechanisms and Factors Contributing to the Development of IBD
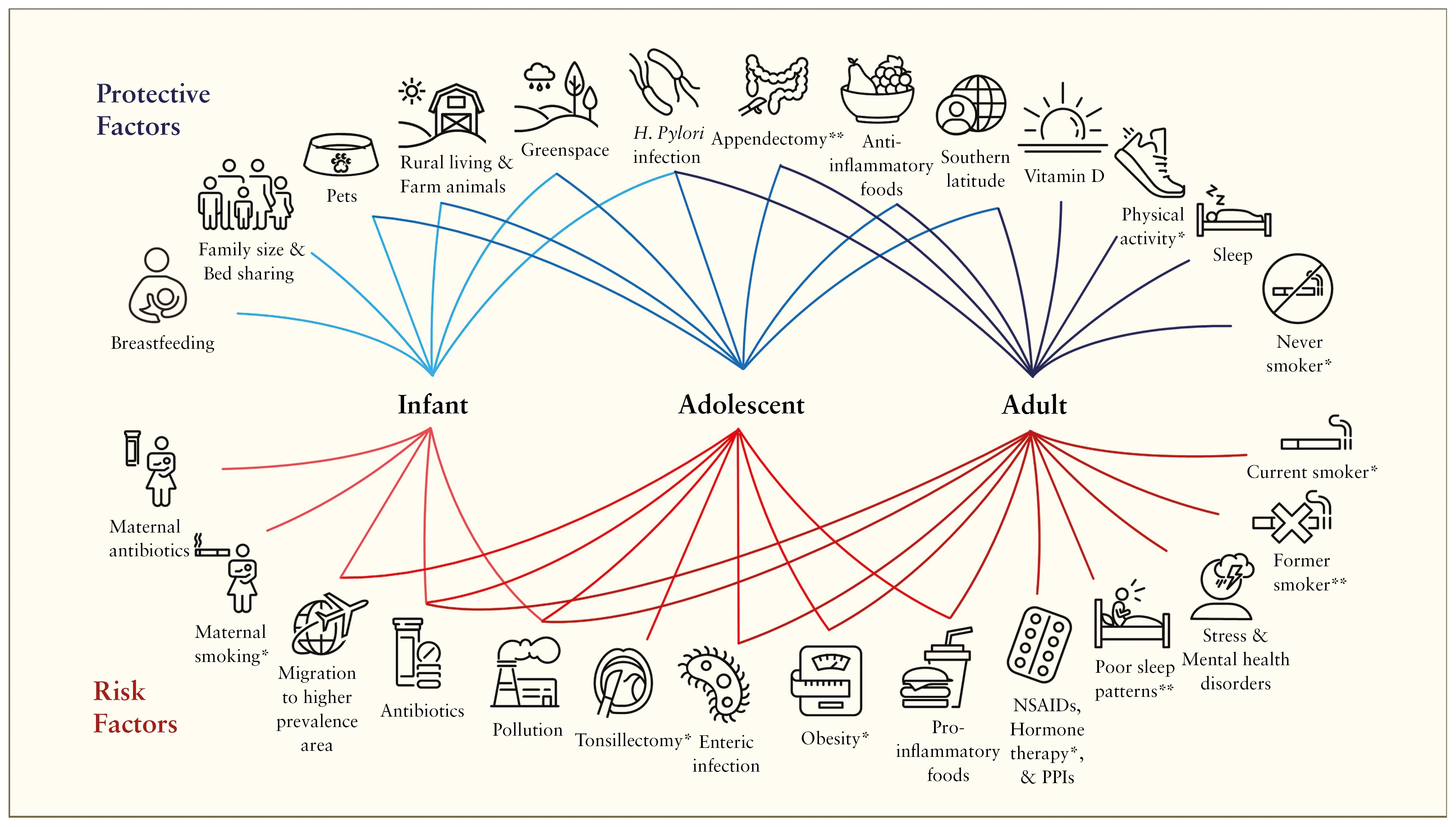
It is not exactly known what causes IBD. It is considered to be due to an interplay of genetics, environmental risk factors (smoking, antibiotic use, diet, early childhood exposures, pollution), an altered intestinal microbiome and dysregulated immune response.
Click on the boxes below to learn more.
Genetic Factors
Although having certain genes can increase your risk for Inflammatory Bowel Disease (IBD), genetics alone don’t determine whether someone will develop it. Researchers have identified over 200 genetic variants (risk “loci”) associated with IBD, 110 of which are shared with CD and UC 6. Many of these are also associated with other immune-mediated diseases like ankylosing spondylitis and psoriasis, which are common extra-intestinal manifestations of IBD.7 Many of these genes influence how the immune system responds, how the lining of the gut works, or how your body interacts with the microbes in your intestines.8
Still, even with all those genetic markers, researchers estimate that these genetic risk factors explain less than 30% of why IBD occurs in people, which means that environmental and other non-genetic factors must play a large role.9
Indeed, over the past several decades, IBD has increased sharply in countries adopting a more “Western” lifestyle, changes in diet, sanitation, antibiotics use, urban living, and other environmental exposures have been strongly linked to that rise.10 Moreover, recent studies suggest that among people who do develop IBD, environmental factors can strongly influence when the disease appears, sometimes even more than genetics. In one large recent study, environmental exposures explained a significant portion of the variation in age at diagnosis of IBD, while genetic risk was not significantly associated with earlier onset.11
In practical terms: having “IBD genes” may raise your susceptibility, but many people who carry risk genes never develop IBD, because in many cases the “triggering conditions” involve changes in environment, diet, gut microbes, or other life exposures. Because environment appears to be such a big piece of the puzzle, this means there is hope, modifying environmental and lifestyle factors may influence not just risk, but potentially the disease course.
Environmental and Lifestyle Factors
Environmental and lifestyle factors play a crucial role in the risk of developing IBD. Diet, physical activity, smoking, and antibiotic use can influence intestinal inflammation and the composition of the microbiome.
- Diet: The Western diet, especially a high intake of highly processed foods and a low-fiber diet, can disrupt the intestinal barrier and promote inflammation.
- Exercise: Physical activity and exercise have been shown to positively influence the diversity of the microbiome.
- Smoking: has an ambiguous effect: it worsens Crohn's disease, but appears to have a protective effect against ulcerative colitis. Obviously, the benefits of potentially preventing ulcerative colitis do not outweigh the other health risks of smoking.
- Antibiotic: use can disrupt the gut microbiome and potentially trigger or worsen IBD symptoms.
Changes in the Gut Microbiome
The gut microbiome is the collection of billions of bacteria, viruses, fungi and other microorganisms that live in the intestines. These microbes play an important role in digestion, the immune system and general health. A healthy balance of the gut microbiome helps digest food, fight harmful invaders and reduce inflammation. It plays a crucial role in maintaining intestinal health. Dysbiosis, or an imbalance in intestinal bacteria, is associated with the development of IBD.

Molecular Mechanisms
At the molecular level, several mechanisms contribute to the development of IBD:
- Intestinal Barrier Dysfunction:
The intestines are lined with epithelial cells, which form a protective barrier between the intestinal contents and the rest of the body. They help with the absorption of nutrients, prevent harmful substances and bacteria from entering the body and play a role in the immune system by sending signals in the event of infections or inflammation. Disruption of this barrier allows the passage of bacteria and antigens, triggering immune responses and inflammation. This is also called intestinal permeability, or leaky gut. - Cytokine production:
Cytokines are small proteins released by cells of the immune system to regulate the immune response. They activate other immune cells to help fight infections and promote wound healing. Some cytokines inhibit inflammation and while other cytokines stimulate inflammation, leading to possible tissue damage and increased inflammation. Inhibiting these cytokines is the basis of many current treatments for IBD. - Oxidative stress:
When there is inflammation in the intestines, the body produces extra aggressive oxygen particles, also called reactive oxygen species (ROS). These particles can cause damage to cells and tissues in the intestine. This is called oxidative stress. This damage weakens the intestinal wall, making it easier for bacteria and other harmful substances to enter. This ensures that the immune system continues to respond and does not stop the inflammation - thus creating a negative vicious circle.13
Diet and Lifestyle in IBD
Diet is an integral component of managing inflammatory bowel disease. Using a tailored nutritional approach as a part of treatment can help manage symptoms, impact inflammation levels, induce/maintain remission and improve quality of life.
Nutritional therapies should be individualized based on disease activity, nutritional status, and personal preferences. Regular monitoring from healthcare providers, including gastroenterologists and dietitians, is essential and ensures that dietary modifications are safe and nutritious.
Other lifestyle changes can also complement medical treatments for IBD and may significantly help improve symptom control and quality of life. A recent study compared standard care with a multimodal lifestyle intervention. This study, with a focus on a healthy diet, stress reduction, sleep and exercise, shows that fatigue in IBD patients in remission significantly improved.14
Explore the links below to learn about how diet and lifestyle can help manage IBD:
- Dietary Options for IBD
- The IBD Nutrition NavigatorTM, a tool to help patients and healthcare providers jointly determine which dietary therapy is the best fit
- Lifestyle articles that complement medical care
Can IBD be Prevented?
Environmental modification strategies are crucial in preventing IBD and reducing its overall societal impact. Observational research has shown the potential for lifestyle and dietary changes to prevent the onset of IBD. While more research is still needed, current available evidence supports the following strategies that may reduce the likelihood of developing IBD.10
Guidance for healthcare providers on reducing the risk of developing IBD based on meta-analyses of observational research studies, while awaiting higher quality interventional and randomized controlled studies of disease prevention10
Breastfeeding
- Offers numerous health benefits to infants and is encouraged when possible
- Breastfeeding for at least 3 months may be more beneficial than for shorter durations
Certain dietary habits may be associated with a lower risk of IBD:
- Lower intake of red meat and higher consumption of fish
- Increase consumption of plant-based foods, including fruits and vegetables
- Maintain the recommended daily fiber intake (>25 g/d)
- Ensure adequate vitamin D intake through diet or supplementation
- Reduce consumption of ultra-processed food
- Prioritize tea consumption while minimizing the intake of soft drinks
- Adopt the Mediterranean-like diet over the traditional Western diet
Optimizing the following lifestyle factors may help prevent IBD:
- Physical activity: Follow the World Health Organization’s recommendations of at least 150 minutes of moderate-intensity aerobic physical activity or 75 minutes of vigorous-intensity aerobic physical activity per week for adults aged 18–64.
- Maintaining a healthy weight: Avoid obesity (defined as a BMI over 30) through regular exercise and healthy eating.
- Mental health: Individuals experiencing depression should seek appropriate treatment.
- Avoid Smoking: In addition to its negative impacts on cardiovascular health and its role as a risk factor for lung disease and numerous other concerns, smoking is also an independent risk factor for developing IBD. Smoking increases the risk of CD, while former smokers are at a higher risk of UC.
Medications
- Proton Pump Inhibitors (PPIs): Avoid excessive use when possible.
- Antibiotics: Use antibiotics as recommended by healthcare providers. However, unnecessary use, particularly in early life, should be avoided.
- Oral contraceptive pills: Consult with a primary care physician on the risks and benefits of oral contraceptive pills compared to alternate forms of contraception.
Although medical treatments play a crucial role in managing IBD, it is clear that the future of IBD management lies in a holistic approach that takes into account the unique needs and circumstances of each patient and optimally combines medication, lifestyle and nutrition. Nutritional therapies offer promising opportunities to support intestinal health and reduce inflammation. However, it is crucial that these treatments are tailored to the individual needs and tolerances of each patient, under the guidance of a healthcare professional.
Authors: Dr. Anje Te Velde, Victorien Madsen, Liz Hoobschaak
Medical Reviewers: Dr. Pieter Stokkers
References
- García-Mateo S., Jesús Martínez-Domínguez S.,et al., Healthy Lifestyle Is a Protective Factor from Moderate and Severe Relapses and Steroid Use in Inflammatory Bowel Disease: A Prospective Cohort Study, Inflammatory Bowel Diseases, Volume 31, Issue 1, January 2025, Pages 95–104, https://doi.org/10.1093/ibd/izae062
- F.Chicco, S.Magrì, et al., Multidimensional Impact of Mediterranean Diet on IBD Patients, Inflammatory Bowel Diseases, Volume 27, Issue 1, January 2021, Pages 1–9, https://doi.org/10.1093/ibd/izaa097
- Rozich JJ, Holmer A, Singh S. Effect of Lifestyle Factors on Outcomes in Patients With Inflammatory Bowel Diseases. Am J Gastroenterol. 2020;115(6):832-840. doi:10.14309/ajg.0000000000000608
- Więcek M, Panufnik P, Kaniewska M, Lewandowski K, Rydzewska G. Low-FODMAP Diet for the Management of Irritable Bowel Syndrome in Remission of IBD. Nutrients. 2022; 14(21):4562. https://doi.org/10.3390/nu14214562
- Wang R, Li Z, Liu S, et alGlobal, regional and national burden of inflammatory bowel disease in 204 countries and territories from 1990 to 2019: a systematic analysis based on the Global Burden of Disease Study 2019 BMJ Open 2023;13:e065186. doi: 10.1136/bmjopen-2022-06518
- Jostins, L., Ripke, S., Weersma, R. et al. Host–microbe interactions have shaped the genetic architecture of inflammatory bowel disease. Nature 491, 119–124 (2012). https://doi.org/10.1038/nature11582
- Ramos GP, Papadakis KA. Mechanisms of Disease: Inflammatory Bowel Diseases. Mayo Clin Proc. 2019;94(1):155-165. doi:10.1016/j.mayocp.2018.09.013
- Loddo I, Romano C. Inflammatory BowelDisease: Genetics, Epigenetics, and Pathogenesis. Front Immunol. 2015;6:551. Published 2015 Nov 2.doi:10.3389/fimmu.2015.00551
- Zhao M, Burisch J. Impact of Genes and theEnvironment on the Pathogenesis and Disease Course of Inflammatory BowelDisease. Dig Dis Sci. 2019;64(7):1759-1769.doi:10.1007/s10620-019-05648-wenesis and Therapy. Nutrition in Clinical Practice, 30(6), 760-779. doi:10.1007/s10620-019-05648-w
- Tarun, Chhibba, et al., Environmental risk factors of inflammatory bowel disease: toward a strategy of preventative health, Journalof Crohn's and Colitis, Volume 19, Issue 4, April 2025, jjaf042, https://doi.org/10.1093/ecco-jcc/jjaf042
- Khakoo NS, BeechamAH, Lyu J, et al. Early Life and Childhood Environmental Exposures, More Than Genetic Predisposition, Influence Age of Diagnosis in a Diverse Cohort of 2952Patients With IBD. Clin Gastroenterol Hepatol. 2024;22(7):1462-1474.e5.doi:10.1016/j.cgh.2024.01.020
- Abegunde AT, Muhammad BH, Bhatti O, Ali T. Environmental risk factors for inflammatory bowel diseases: Evidence based literature review. World J Gastroenterol. 2016 Jul 21;22(27):6296-317. doi: 10.3748/wjg.v22.i27.6296. PMID: 27468219; PMCID: PMC4945988.
- Sandys, O., Stokkers, P.C.F. & te Velde, A.A. DAMP-ing IBD: Extinguish the Fire and Prevent Smoldering. Dig Dis Sci70, 49–73 (2025). https://doi.org/10.1007/s10620-024-08523-5
- Loveikyte R., Koppelman L., et al., Multimodal Lifestyle Intervention Improves Fatigue in Quiescent Inflammatory Bowel Disease: A Controlled Study, Crohn's & Colitis 360, Volume 7, Issue 1, January 2025, otaf009, https://doi.org/10.1093/crocol/otaf009
Further Reading & Helpful Tools

Join Our Community
Become a member to save recipes, receive relevant GI nutrition resources and stay updated on new tools, events and education.


