Low-FODMAP Diet
Used for IBS and IBS-like symptoms in IBD as a short-term elimination diet to manage GI symptoms and support long-term food tolerance


About Low-FODMAP
The low FODMAP diet is an evidence-based nutrition approach used to help manage gastrointestinal (GI) symptoms such as bloating, abdominal pain, gas, diarrhea, and constipation.
It is most commonly recommended for people with irritable bowel syndrome (IBS) and may also benefit individuals with inflammatory bowel disease (IBD) who experience IBS-like symptoms, particularly when IBD is in remission.
The low FODMAP diet is not intended to be followed long term. It is a structured, short-term learning process designed to help identify personal food triggers and support symptom-guided nutrition choices.1
Who May Benefit from a Low FODMAP Diet
Because the diet is restrictive, it is best followed with guidance from a registered dietitian, especially for those with IBD, children, or individuals at risk for inadequate nutrition.
What are FODMAPs?
FODMAPs are small-chain carbohydrates (sugars and fibers) that are poorly absorbed in the small intestine2 and can trigger GI symptoms in some individuals.
These carbohydrates can draw water into the intestine and be rapidly fermented by gut bacteria, leading to gas, bloating, pain, and changes in bowel habits.
FODMAPs are found in common foods such as wheat-based products, legumes, some dairy products, certain fruits and vegetables (including apples, pears, onions, garlic, and cauliflower), sweeteners, and some medications.
Low-FODMAP Foods
High-FODMAP Foods
- Eggplant, green beans, bok choy, bell pepper, carrot, cucumber, lettuce, potato, tomato, zucchini
- Cantaloupe, grapes, kiwi, orange, pineapple, strawberries
- Almond milk, brie and camembert cheese, feta cheese, hard cheeses, lactose-free milk, soy milk (made from soy protein)
- Eggs, firm tofu, plain cooked meats/poultry/seafood, tempeh
- Corn flakes, oats, quinoa flakes, quinoa/rice/corn pasta, rice cakes (plain), sourdough spelt bread, wheat-/rye-/barley-free breads
- Dark chocolate, maple syrup, rice malt syrup, table sugar
- Macadamias, peanuts, pumpkin seeds, walnuts
- High in Fructose
- Apples, pears, mangoes, cherries, figs, nashi pears, pears, watermelon, dried fruit
- High in Fructans
- Artichoke, garlic, leek, onion, spring onions
- High in Galacto-oligosaccharides (GOS)
- Red kidney beans, split peas, falafels, baked beans
- High in Fructans and Galacto-oligosaccharides (GOS)
- Wholemeal bread, rye bread, muesli containing wheat, wheat pasta, rye crispbread
- Cashews, pistachios
- High in Mannitol
- Mushrooms, cauliflower, snow peas
- High in Lactose
- Soft cheeses, milk, yogurt
- High in Polyols
- Honey, high fructose corn syrup, artificial sweeteners
What is the Low FODMAP Diet?
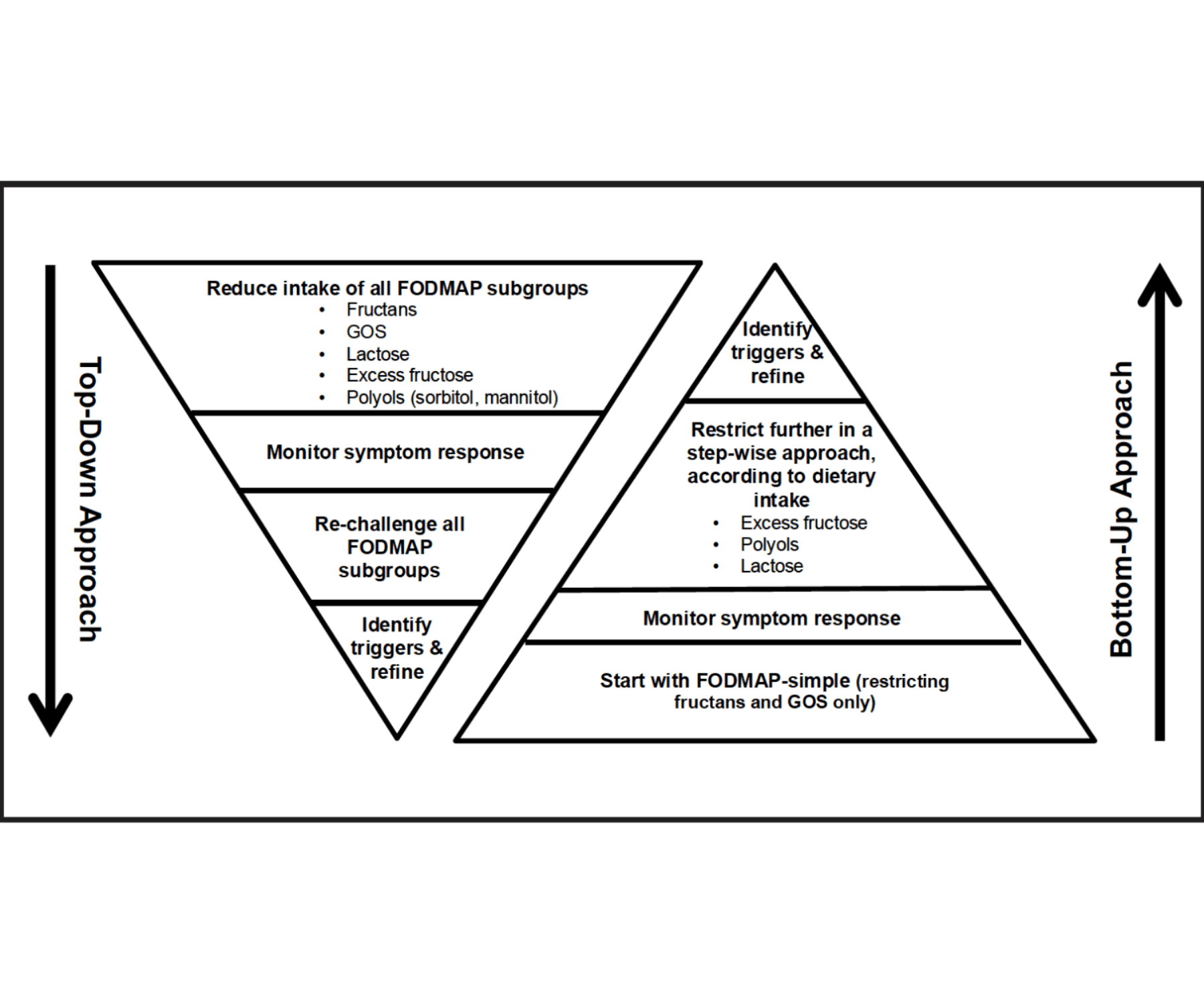
The Low-FODMAP diet (also named the top-down approach) is a 2-6 week elimination diet that involves removing high-FODMAP foods to help you identify your personal dietary triggers. Low-FODMAP is a learning diet rather than one you stay on forever.
This 3-phase strict elimination diet reduces small, commonly malabsorbed carbohydrates that pull water into the small intestine like a water balloon and are fermented by gut microbes, creating gas like a hot air balloon ready for takeoff.3,4
Emerging science also shows that a high FODMAP diet causes mast cell activation (a type of white blood cells in the gut), which in turn leads to colonic barrier loss.5,6
The traditional low FODMAP diet follows a three-phase approach:

Why Small Amounts Can Still be a Problem
Even if you tolerate small amounts of individual high-FODMAP foods, multiple FODMAP sources eaten together, or close in time, can stack up and trigger symptoms.
In other words, it’s not just what you eat but, how much, how many, or how close together in time high-FODMAP foods are eaten.
For example, you might tolerate:
- a small serving of wheat bread
- a small serving of onion
- a small serving of apples
But eating all three in the same meal may lead to symptoms. Each individual fills their bucket differently, so tolerance to FODMAP-rich foods can vary from one person to another.
Low-FODMAP and IBS
The Low-FODMAP diet is one of the most studied dietary therapies for IBS:

Low-FODMAP and IBD
More than 30% of people with IBD in remission experience IBS-like symptoms. While the low FODMAP diet does not improve IBD disease activity or reduce fecal calprotectin, it may help decrease global digestive symptoms and improve quality of life when intestinal inflammation is well controlled.10 For individuals with IBD, the low FODMAP diet may be used to manage persistent functional GI symptoms attributed to IBS rather than active inflammation, but it is not a dietary treatment for IBD itself.
A Low-FODMAP diet can be difficult to implement properly. Patients, especially those with IBD, should consult with an experienced dietitian. A Low-FODMAP Diet may not be a good choice for everyone, particularly for those at risk of developing eating disorders.
Fiber-containing foods should be added slowly and in small quantities to allow the body to adapt to processing more fiber and build the proper muscles and bacteria to handle fiber. For patients who are not currently consuming many fiber-containing foods, adding in high-FODMAP foods could cause gastrointestinal symptoms due to the fiber rather than the carbohydrates. High-FODMAP foods draw water into the intestines, which can perpetuate diarrhea. The fermentation of high-FODMAP foods by bacteria in the colon can cause bloating, gas, and cramping pain.
Excessive fiber intake from fruits and vegetables can cause GI pain and an increased risk of a bowel obstruction, particularly in patients with strictures. Patients with strictures should take extra care to first peel fruits and vegetables, cook them well and may need to consider pureeing them initially.
If a Low-FODMAP diet is not right for you, other options for treating persistent symptoms are a Gluten-free, Dairy-Free and/or Lactose-Free Diets or avoiding Trigger Foods.
Important Considerations When Following a Low-FODMAP Diet
The Low-FODMAP diet11:
- Can be challenging and restrictive, especially during elimination
- Requires careful reintroduction to avoid unnecessary long-term restriction
- May temporarily alter the gut microbiota if followed without personalization
The low FODMAP diet and other exclusion diets should be used with caution or avoided in individuals who11:
- Are already highly restricting food without symptom improvement
- Have a history of disordered eating or avoidant restrictive food intake
- Are unable to reintroduce foods safely
The FODMAP Gentle Diet
A Less Restrictive Option
The FODMAP Gentle diet (also named the "bottom-up" approach) is a more liberal restriction of FODMAP carbohydrates based on patient's clinical history and diet intake. It is less studied than the traditional low FODMAP diet with symptom benefits based on clinical observations.
Clinical observation and two small human studies reveal that not all FODMAPs are created equally, with fructans, galactans, and mannitol associated with worsening of abdominal pain and/or bloating.12,13
A limited-low FODMAP diet that eliminates only fructans and galacto-oligosaccharides was as effective as a standard low-FODMAP diet.14
Who May Benefit from a Gentle FODMAP Diet?15
Key Takeaways
Working with a knowledgeable dietitian can help ensure the approach is safe, effective, and nutritionally balanced.
References
- Cox SR, Lindsay JO, Fromentin S, et al. Effects of Low FODMAP Diet on Symptoms, Fecal Microbiome, and Markers of Inflammation in Patients With Quiescent Inflammatory Bowel Disease in a Randomized Trial. Gastroenterology. 2020;158(1):176-188.e7. doi:10.1053/j.gastro.2019.09.024
- Singh P, Tuck C, Gibson PR, et al. The role of food in the treatment of bowel disorders: focus on irritable bowel syndrome and functional constipation. Am J Gastroenterol. 2022; 117(6):947-957. doi: 10.14309/ajg.0000000000001767.
- Spencer M, Chey WD, Eswaran S. Dietary renaissance in IBS: has food replaced medications as a primary treatment strategy? Curr Treat Options Gastroenterol. 2014; 12(4):424-40. doi: 10.1007/s11938-014-0031-x.
- Haller E, Scarlata K. Diet interventions for irritable bowel syndrome: separating the wheat from the chafe. Gastroenterol Clin North Am. 2021; 50(3):565-579. doi: 10.1016/j.gtc.2021.03.005. Reprinted with permission from Elsevier.
- Singh P, Grabauskas G, Zhou SY, et al. HighFODMAP diet causes barrier loss via lipopolysaccharide-mediated mast cellactivation. JCI Insight. 2021; 6(22):e146529. doi: 10.1172/jci.insight.146529.
- Gao J, Lee AA,Abtahi S, et al. Low fermentable oligosaccharides, disaccharides,monosaccharides, and polyols diet improves colonic barrier function and mastcell activation in patients with diarrhea-predominant irritable bowel syndrome:a mechanistic trial. Gastroenterology. 2025. doi:10.1053/j.gastro.2025.07.016.
- Black CJ, Staudacher HM, Ford AC. Efficacy of a low FODMAP diet in irritable bowel syndrome: a systematic review and network meta-analysis. Gut. 2022; 71(6):1117-1126. doi: 10.1136/gutjnl-2021-325214.
- Dean G, Chey SW, Singh P, et al. A diet low in fermentable oligo-, di-, monosaccharides and polyols improves abdominal and overall symptoms in persons with all subtypes of irritable bowel syndrome. 2024; 36(8):e14845. doi: 10.1111/nmo.14845
- Carbone F, Van den Houte K, Besard L, et al. Diet or medication in primary care patients with IBS: the DOMINO study - a randomised trial supported by the Belgian Health Care Knowledge Centre (KCE Trials Programme) and the Rome Foundation Research Institute. Gut. 2022; 71(11):2226-2232. doi: 10.1136/gutjnl-2021-325821.
- Ville A, McRae R, Nomchong J, et al. Effects ofa Low FODMAP Diet in Inflammatory Bowel Disease and Patient Experiences: AMixed Methods Systematic Literature Review and Meta-Analysis. J HumNutr Diet. 2025;38(4):e70106. doi:10.1111/jhn.70106
- Prados A. The low FODMAP diet can pose challenges for people with IBS. What can be done to minimize some of those challenges in clinical practice? European Society of Neurogastroenterology & Motility. Available from: https://www.gutmicrobiotaforhealth.com/the-low-fodmap-diet-can-pose-challenges-for-people-with-ibs-what-can-be-done-to-minimize-some-of-those-challenges-in-clinical-practice
- Eswaran S, Jencks KJ, Singh P, et al. AllFODMAPs aren’t created equal: results of a randomized reintroduction trial inpatients with irritable bowel syndrome. Clin Gastroenterol Hepatol.2025; 23(2):351-358.e5. doi:10.1016/j.cgh.2024.03.047.
- Van den Houte K, Colomier E, Routhiaux K, et al. Efficacy and findings of a blinded randomized reintroduction phase for the low FODMAP diet in irritable bowel syndrome. Gastroenterology. 2024; 167(2):333-342. doi: 10.1053/j.gastro.2024.02.008.
- Singh P, Chey SW, Nee J, et al. Is a simplified, less restrictive low FODMAP diet possible? Results from a double-blind, pilot randomized controlled trial. Clin Gastroenterol Hepatol. 2025; 23(2):362-364.e2. doi: 10.1016/j.cgh.2024.04.021.
- Halmos EP, Gibson PR. Controversies and reality of the low FODMAP diet for patients with irritable bowel syndrome. J Gastroenterol Hepatol. 2019; 34(7):1134-1142. doi: 10.1111/jgh.14650.
- Scarlata K. Gentler solutions: adapting the low FODMAP elimination diet for irritable bowel syndrome for symptom relief. Pract Gastroenterol. 2025;49(9) Available from: https://practicalgastro.com/2025/09/15/gentler-solutions-adapting-the-low-fodmap-elimination-diet-for-irritable-bowel-syndrome-for-symptom-relief/
Low-FODMAP Research articles
Delicious and Nutritious Recipes
Explore all recipesOur recipe section offers a wide range of options that align with various nutritional therapies, ensuring you can find meals and snacks that are both flavorful and supportive of your dietary needs.
Additional Low-FODMAP Resources




Support our Mission
Your donation will help us to enhance the well-being and health outcomes of patients with GI conditions.
Donate


.webp)

